
|
|
|||||
|
|
|
|
|
|
|
QuickScroll Case 1 | Case 2 | Case 3 | Case 4
Look at this patient's skin and proceed!
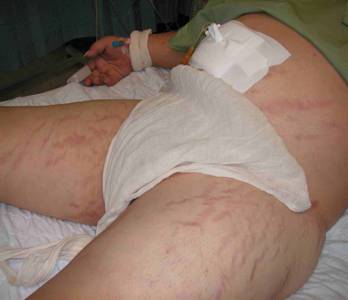
Discussion:
It is a common case in MRCP station 5 of endocrine sub- station. There is presence of obvious purplish striae over his abdomen as well as his upper thigh. Check for other obvious clinical signs such as buffalo hump, moon face, thin skin, multiple bruises especially over venesection site, hirsutism and acne. Look for proximal myopathy and spine tenderness. Suggest to examiners that you would like to do the following, check the urine for glycouria, check this patient’s BP and ask relevant history to assess whether the patient is on long term steroid. Look at his abdomen to see any surgical scar.
Conclusion:
This gentleman has Cushing’s syndrome secondary to long term steroid ingestion ( from traditional medicine). He was admitted due to fulminant sepsis with Addisonian crisis.
Extra points:
- Common diseases that requires patients on long term steroid are as asthma, myasthenia gravis, nephrotic syndrome and other autoimmune diseases.
- Cushing’s disease is always a common case in exam, remember that besides making the diagnosis of Cushing, you need to find out the underlying cause if possible and possible complications.
| Case ID: 2 | Created: 29 May 2006 |
Station 4:
You are the SHO in charge of the medical clinic
Dear Dr,
Mrs Lydia David, a 70-year old retired teacher comes to your clinic because of jerky movement of her right hand for the past four months. She has previous history of Diabetes Mellitus on oral medications under her GP follow up. After a careful physical examination and complete investigations, your consultant neurologist thinks that Mrs Davis is suffering from Parkinson’s disease. Mrs David is in the clinic waiting to see you for the investigation results and the diagnosis. You are the SHO in charge of the neurology clinic, your task is to explain to Mrs David about the diagnosis and answer her queries.
You have 14min until the patient leaves the room, followed by 1min for reflection before the discussion with the examiners. Be prepared to discuss the solutions to the problems posed by the case and how you might reply the GP’s letter.
Conclusion:
This is a classical question that can be asked in your counselling station. I call this type of question, “Disease explanation” question, other diseases that are common in the exam include Alzheimer’s disease, Motor neuron disease, Hepatitis B and C , polycystic kidney disease ……..etc. Usually all these diseases are chronic or they have a lot of social implications. In this case, since that Mrs Davis is suffering from Parkinson’s disease, candidates are expected to do the following,
- to explain the illness in layman's terms,
- explain the prognosis and the likely progression of the illness,
- treatment for the disease- medical or any new treatment available such as surgical intervention,
- ask social history especially the impact of the illness towards patient’s daily activities as well as patient’s relationship with other family members.
Extra points:
- The commonest mistake candidates make in this type of question is trying to explain as much as possible about a illness and not answering patient’s queries about the illness,
- Try to give a lot of details about the illness and not bother about the illness social implication.This gives an impression to the examiners that you are not holistic in your approach.
| Case ID: 3 | Created: 29 May 2006 |
This patient complains of double vision, would you like to examine him.
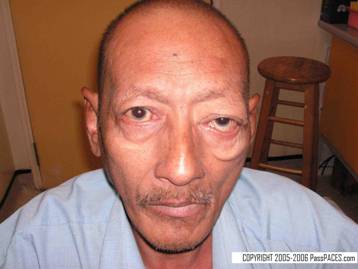
Discussion:
Ptosis is always a popular question in MRCP PACES, this gentleman has left unilateral partial ptosis. After you notice this, there are two common possibilities, either the patient is suffering from left Horner’s syndrome or left third nerve palsy. The second step you would like to do is of course to look at the affected eye’s pupil size. This will tell you whether you are dealing with a third nerve palsy or Horner’s syndrome. If the pupil’s size is small then you are dealing with Horner’s or else you are dealing with third nerve palsy especially you notice that the eye is abducted.
Conclusion:
This patient has left isolated third nerve palsy due to diabetes mellitus.
Extra points,
- Common question examiners will ask you is the reason behind pupillary sparing in ‘medical’ third nerve palsy.
- Sometimes (rarely) you may think that the patient has ptosis but what the patient is having is unilateral proptosis due to retroorbital tumour/ mass
| Case ID: 4 | Created: 29 May 2006 |
Look at this patient and proceed.

Discussion:
It is sometimes rather difficult for you to differentiate panhypopituaitarism from hypothyroidism. However, if you look at patient’s sexual characteristics, they are lost in in panhypopituitarism .Patients with hypothyroidism also tend to be older because the main cause for panhypopituitarism is mainly due to Seehan’s syndrome and skull radiation which is commoner among younger patients. Always remember to look for cerebellar signs which is bilateral in hypothyroidism. Also look for other associated endocrine involvement such as DM, Addison’s disease, Pernicious anemia and vitiligo. Suggest to examiners you would like to check for sensory deafness especially to high tone. Try to find out the underlying cause for the hypothyroidism if possible.
Conclusion:
This lady has hypothyroidism secondary to previous total thyroidectomy.
Extra points:
1)Although it is rather uncommon in PACES, you can find this illness rather common especially among older population. Always check their thyroid status if an elderly patient presents to you with dementia.
2)The commonest cause for hypothyroidism is previous total thyroidectomy.
To see the previous issues, click here! To send a quick comment, use our shoutbox, click here!
Source:
1) Handbook of Current Daignosis and Treatment, Roy Pounder
2) 250 Cases in Clinical Medicine, R R Baliga
(Last modified: 22 October 2006)