
|
|
|||||
|
|
|
|
|
|
|
![]()
YOUR LATEST ISSUE ABOUT MRCP PACES IS HERE!
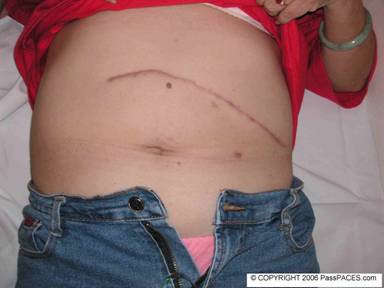
This lady complains of lethargy, would you like to examine her abdominal system?
Discussion:
In MRCP exam, if you encounter a surgical scar, it is always a good start because surgical scar can give you a lot of clues that lead to possible underlying diagnosis. This lady has a roof-top scar ( can be just a horizontal scar at left lumbar region) and further examination reveals jaundice, moderate hepatomegaly but no stigmata of chronic liver disease ( always look for stigmata of chronic liver disease, due to her illness , she needs multiple transfusions and tend to get Hepatitis B and C in long run and possibility of liver cirrhosis due to iron overload) . Look hard for any multiple small scars at the abdomen due to subcutaneous infusion of iron-chelation therapy.The underlying diagnosis for this lady with chronic haemolysis is Thalassemia with previous splenectomy. Although Thalassemia is rather uncommon in UK, it is common in Asia especially if you are sitting your exam in Singapore, Hong Kong and Malaysia. Suggest to examiners you would,
- Examine for secondary sexual characteristics ( any hypogonadism)because there is possibility of delayed puberty due to iron overload
- Check for patient’s height due to growth retardation secondary of iron deposition at the pituitary gland
- Check urine for diabetes mellitus
- Look for signs of hypothyroidism (all these are due to iron overload)
- Ask the patient any family history of anemia and Haemoglobinpathy.
There are in various occasions my friends got a abdominal case of isolated mild splenomegaly and tinge of jaundice without hepatomegaly in their MRCP PACES, always remember one of the most important causes is chronic haemolysis ( although book always tells you that you tend to get hepatomegaly as well, but I notice Thalassemia intermedia patients tend to get splenomegaly ONLY).
Conclusion:
This lady has Thalassemia Major and underwent a splenectomy due to recurrent, frequent transfusions.
Extra points,
a)Splenectomy should be considered if,
- annual blood requirements exceed 1.5 times those of spenectomised patients, provided they are on the same transfusion scheme and have no other reasons for increased consumption.
- Splenic enlargement is accompanied by symptoms such as left upper quadrant pain and early satiety.
- Leucopenia or thrombocytopenia due to hypersplenism.
b) Complications of splenectomy include peri-operative complications such as bleeding,atalectasis and subphrnic abscess, long term complications include thrombocytosis and overwhelming sepsis especially to encapsulated organisms such as Streptococcus pneumonia, Haemophilus influenzae and Neiserria meningitides.
c) Preventive measures a physician can utilize to prevent postsplenectomy sepsis include immunoprophylaxis ( vaccination to S.pneumonia, H.influenzae and N.meninngitidis), chemoprophylaxis ( oral penicillin) and patient education (explain about potential travel-related infections)
| Case ID: 2 | Created: 4 June 2006 |
Station 2: You are the SHO in charge of the medical unit.
Dear Dr,
Ref: Mr David Letterman, 56 years old
Thank you for seeing Mr Letterman who complains of lethargy for the past 3 months. I have done a few investigations that turned out to be negative. He has previous history of gastritis and claimed that OGDS done about 5 years ago showed some erosions and he was put on some medications.
He has history of Diabetes Mellitus for the past 10 years currently on T Daonil 5mg bd. He is worried about his symptoms but unfortunately I can’t find anything wrong with him.
Kindly see him and advise.
With best wishes,
Dr GP
You have 14min until the patient leaves the room, followed by 1min for reflection before the discussion with the examiners. Be prepared to discuss the solutions to the problems posed by the case and how you might reply the GP’s letter.
Discussion:
You must always think of possible differential diagnosis before you enter the examination room. Mr Letterman complains of lethargy, a very vague symptom. You must start off by asking him what does he mean by lethargy. Common causes of lethargy/tiredness can be due to anemia, hypothyroidism, depression, myathenia gravis, obstructive sleep apnoe. You must ask him to explain his symptom. Some patients may associate shortness of breath with lethargy. In whatever symptoms you are going to encounter in MRCP PACES,always try to include these questions in your history-taking if possible,
![]() any specific time the symptom becomes worse? If the patient is having mysthenia gravis, he may tell you that he fells more tired especially during evening,
any specific time the symptom becomes worse? If the patient is having mysthenia gravis, he may tell you that he fells more tired especially during evening,
![]() any precipitating or relieving factors?
any precipitating or relieving factors?
![]() any other associated symptoms?
any other associated symptoms?
In this case, you must ask certain questions which are specific for hypothyroidism such as constipation, weight gain, cold intolerance. You need to rule out causes of anemia as well since that this gentleman had a history of gastritis before. Ask about any symtoms to suggest blood loss or symptoms to suggest malignancy. Depression is always a differential in your history taking, try to assess his social history and symptoms to suggest depression. In obstructive sleep apnoe, patient may have snoring, early morning headache and sleepiness during day time. As I mentioned earlier, myathenia gravis patients always tell you that their symptoms worsen towards the evening.
About his diabetes, you must always ask the following,
![]() his usual control, whether he has monitoring at home to monitor his sugar,
his usual control, whether he has monitoring at home to monitor his sugar,
![]() possible complications such as IHD, retinopathy, peripheral neuropathy, nephropathy ,TIA, stroke etc,
possible complications such as IHD, retinopathy, peripheral neuropathy, nephropathy ,TIA, stroke etc,
Later, ask other relevant past history, such as in this case, ask the patient about his OGDS and his symptoms.
Last but not least, always assess patient's main concern, he may have some hidden agendas that he like to tell you. Actually, my friend had this case in his MRCP PACES in 2005, the diagnosis was depression. My friend totally forgot to ask the patient about his social history. This patient actually just lost his wife in a motor vehicle accident and he had very poor social support and he developed depression after the incident!
To see previous issues, click here! To send a quick comment, use our shoutbox, click here!