
|
|
|||||
|
|
|
|
|
|
|
 |
|
|||
| Your latest issue for MRCP PACES is here! |
Would you like to examine this lady's hands?
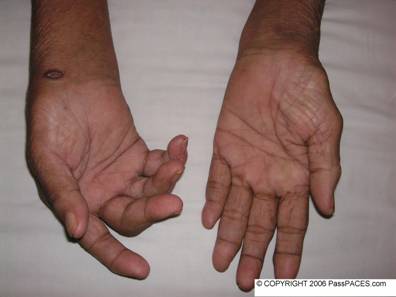
Discussion:
You may be panic when you first look at her hands. Always remember the general rules for a good physical examination for locomotor system, i.e inspect, feel, palpate, passive movement, functional assessment and special steps! Always remember that “NEVER SHAKE HAND WITH PATIENT!” in locomotor sub-station. ( but for neurology station, always do this first!) . You may cause pain to patient and examiners have 1 thousand and 1 reason to fail you! Always ask you patient whether he/she has any pain over any specific joint, then I would ask them to rest their hands on a pillow. Second rule is proper exposure, preferably I would ask patient to expose the whole upper limbs up to shoulder, the reason is simple, you do not want to miss any skin rash ( especially psoriasis patch) , any skin nodule ( especially subcutaneous nodule over the elbow in rheumatoid arthritis ) and any abnormal joint deformity. Describe any abnormality you can see such as joint deformity, muscles wasting … etc. Do a proper inspection! What I mean, look over patient’s palm as well as the back of the hand. If you do so…………
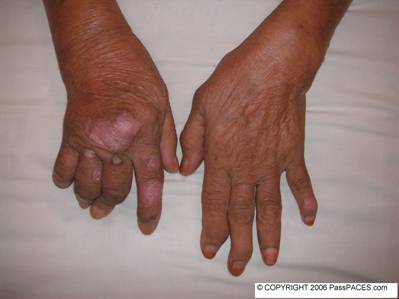
Ops……, the diagnosis becomes obvious after turning the patient’s hand. Another important inspection I would pay attention to is whether there is presence of nail pitting. After general inspection, then feel the patient’s skin gently to assessment whether there is presence of warmness that might suggest disease activity. Then palpate the patient’s joints by gentle passive movement and look for any thickening of synovium or joint tenderness. Also try to feel for calcinosis that might be present in scleroderma. I would always tap at patient’s flexor retinaculum to check for carpal tunnel syndrome. The last step is assessing patient’s functional status. Do at least these three important steps, unbuttoning of clothes, pincer grip ( holding key) and writing. If you suspect there is involvement of elbow and shoulder joints, then ask patient to comb his/her hair. You can kill two birds with one stone by asking patient to do so. You are going to assess patient’s elbow as well as shoulder joints. Then the last step will be special steps depending on your findings. Such as in this case, I would suggest to examiners that I would look for other joints involvement and other common sites for psoriasis.
Common questions examiners would ask you,
- Why in arthritis mutilans, there is shortening of the fingers ?( due to marked periarticular osteolysis and erosion)
- What is ‘pencil in a cup’ appearance in xray?
- Where are the common sites to find psoriatic patches?
- How would you manage psoriatic arthropathy?
Conclusion:
This lady has psoriatic arthropathy.
Extra points:
- Five types of psoriatic athropathy namely oligoarticular asymmetrical type (70%), distal interphalangeal type, rheumatoid arthritis-like ( common in exam because want to confuse you!), ankylosing spondylitis- like and arthritis mutilans!
- There are five types of psoriasis. They are chronic plaque, inverse psoriasis, pustular, guttate and erythrodermic types. (Facts from Baliga's book!)
| Case ID: 2 | Created: 9 June 2006 |
Examine this gentleman's cardiovascular system.
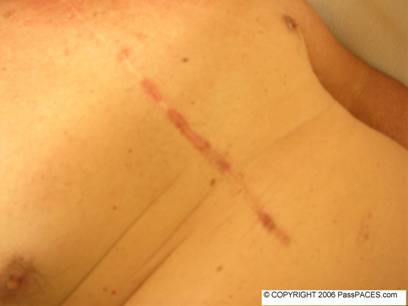
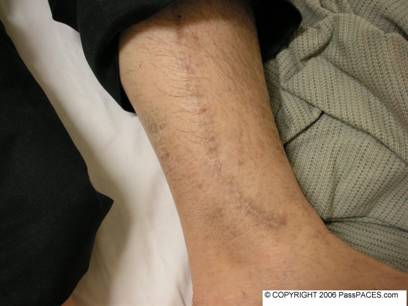
Discussion:
Patients with scars again! I want to show you this case for a simple reason. There are only a few common causes of a sternotomy scar in CVS station. These causes include previous bypass surgery, valve replacement and correction of congenital heart diseases such as VSD ( ventricular septal defect) and ASD ( atrial septal defect). At the first look, you might think that these patient has had a bypass surgery before due to the scar over his leg. The problem is he actually has a bypass and aortic valve replacement (AVR) surgery done before. Lesson to be learned here is always look for concomitant AVR if patient has had a bypass before especially in elderly population because aortic stenosis is common among this age group. During your examination, always look hard for any bruises to suggest over-warfarinization, signs to suggest endocarditis and murmurs to suggest valve dysfunction.
Common questions examiners would ask you,
- Complications of mechanical prosthetic valve. ( can be divided into complications due to the valve itself such as dysfunction, haemolysis, endocarditis….. and complications due to the treatment because of warfarin.)
- Causes of anemia in a patient with prosthetic valve.
- How to differentiate a tilting disc valve from a ball cage valve clinically? (distinction question!)
- How to assess whether the valve is functioning well clinically?
- You can’t find any donor site and no mechanical click when you examine the patient but you see a sternotomy scar, you might be dealing with previous corrective surgery due to congenital heart or a BIO-PROSTHETIC VALVE!
- Although patients with valve repairs tend to have left thoracotomy scar ( such as in mitral stenosis), I found out some patients may have sternotomy scar!
Conclusion:
This gentleman has AVR surgery done before due to previous aortic stenosis and bypass surgery.
Extra points,
To see previous issues, click here! To send a quick comment, use our shoutbox, click here!